media library
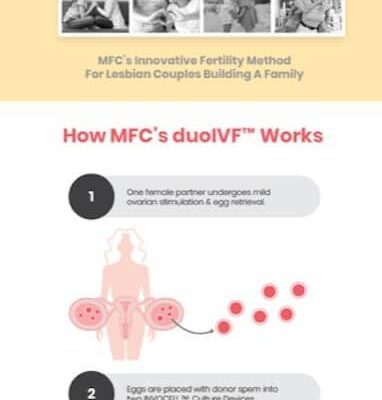
Your comprehensive resource guide for all things related to fertility and reproductive health. Dive into a wealth of carefully curated media including educational videos, blogs, articles and informative guides designed to empower you with knowledge about the journey through fertility diagnostics and treatments.

faq
Welcome to our treatment FAQ section, your go-to resource for answers to real-world questions about fertility and fertility treatments. Whether you’re curious about the basics, want a “big-picture” overview or just want more insight into the experience, we’ve got you covered.

fertility lexicon
A glossary of terms related to fertility and reproductive health. Whether you’re a seasoned expert or just beginning your journey, our lexicon provides clear definitions of key medical terminology that can help you better understand your fertility journey.

ask dr. uzelac
Have a question that you can’t find the answer to? Ask Dr. Uzelac and he’ll answer it during The Infertiligence Podcast.
faq
Fertility
Clinic
What is infertility?
What causes infertility?
What are my chances of getting pregnant at home?
How common is miscarriage?
What fertility testing do I need?
Does fertility testing hurt?
How can I get the above fertility completed?
How do you approach (fallopian) tubal evaluation?
What is IVF?
How long does IVF take?
Does IVF hurt?
Which is better: a fresh or a frozen embryo transfer?
What are the success rates of IVF?
What is embryo banking?
Can I go through IVF as a single parent?
Lab
Where is our IVF lab located?
What hormone tests do I need as part of an infertility evaluation?
What information does a semen analysis provide?
Can my partner do double collections for IUIs?
How do you process sperm for use with IUI or IVF?
What fertilization techniques do you use, ICSI or conventional insemination?
What kind of embryo culture system do you use?
In addition to helping me to become pregnant, what else can I learn from going through IVF?
Should I choose preimplantation genetic testing for aneuploidy (PGT-A) as part of my IVF lab plan?
What other genetic technologies do you offer besides PGT-A?
What is your policy on working with abnormally fertilized eggs?
How do you ensure no mix ups in the lab?
How long can embryos be frozen?
What makes your lab different?
Is the lab accredited by any professional bodies?
What certifications and experience do your embryologists have?
Egg Freezing
Lab
Is there any way to tell me about the quality of my eggs?
What other information do I get about my eggs in the laboratory?
What is MFC’s “no egg left behind” policy?
What technology and methods do you use for freezing and thawing eggs?
Where are my eggs actually stored?
How long has the lab been performing egg freezing procedures?
How long can eggs be stored once they are frozen?
What are the success rates of egg survival after thawing?
What happens during the thawing process in the lab?
How do they ensure each patient’s eggs are correctly identified and stored?
Are my eggs safe in storage?
What protocols are in place in case of power outages?
What protocols are in place in case of an earthquake?
Clinic
What is ovarian reserve and how do I assess it?
What is egg freezing?
Why would I want to pursue egg freezing?
Does egg freezing affect my future fertility?
How many eggs should I freeze for the future?
Is there an ideal time to freeze my eggs?
I’m still in my 20s. Should I consider egg freezing?
Is there a way to predict how many eggs I might be able to freeze in a single cycle of egg freezing?
What if I don’t reach my egg number goal in a single egg freezing cycle?
Do I have to come off of my birth control?
In the future, do I use my frozen eggs or try to conceive at home first?
What if I don’t end up using my frozen eggs?
How is egg freezing different from IVF?
Can I do both egg freezing and IVF at the same time?
Ovarian Stimulation and Egg Retrieval
Both IVF and Egg Freezing require two identical components to treatment: ovarian stimulation and egg retrieval. Information in the following section applies to both IVF and egg freezing.
Treatment Experience
What are the basic steps to ovarian stimulation/egg retrieval?
- Hormone Stimulation: 10-14 days of hormone injections, ending with a final “trigger shot” 35-36 hours before the egg retrieval. During this time there are typically 4 office appointments for the purposes of “monitoring” (each appointment consists of an ultrasound and blood work to check in on the progress of follicle growth.
- Egg Retrieval: A 20-minute procedure performed under sedation (I.V. anesthesia only, neither intubation nor paralysis). The entire process typically requires a total of 5 office visits.
Is the process safe?
What is a typical monitoring visit like?
What is the purpose of monitoring?
How often will I need to visit the clinic during stimulation?
Can other members of my family join me during appointments?
Do I have to do all the injections myself?
How will I feel during ovarian stimulation?
What medications are used for ovarian stimulation?
How do I prepare for egg retrieval?
What is the egg retrieval like?
What is recovery from egg retrieval at home like?
Can I resume normal activities after egg retrieval?
Lifestyle
How will going through ovarian stimulation and egg retrieval fit into my life?
How should I eat during the process?
What about dietary supplements and vitamins?
Do I have to give up caffeine?
Is alcohol allowed?
Can I still exercise?
Can I continue having sex during treatment?
Is traveling permitted?
Are hot tubs, saunas and pools okay to use?
What about acupuncture and massage?
Fertility lexicon
aneuploidy
antimullerian hormone (AMH)
antral follicle count
assisted reproductive technology (ART)
ask dr. uzelac

Do you have question you want to ask Dr.Peter Uzelac? Whether its about fertility, IVF laboratory or anything related to human reporduction. He is all ears.
The infertiligence podcast isn’t a live-call in show, so we don’t accept phone calls. but you can an audio question on this page and submit to Dr. Uzelac.
During each episode, we’ll choose a question, play it during the show and Dr. Peter Uzelac will reply. To submit your question, all you need is an internet connection and microphone.
But Wait! Be sure to read these four rules first!
1 Use a good microphone
The built in mic on your iPhone, laptop or desktop computer should suffice, but if you have an external microphone, even better. We prefer higher quality calls over scrathrty ones
2Make it 30 second or less
Your question should be shortly and snappy. The software only record the first 30 second.
3State your first name and location
Start your call by telling us who you are and where you’re from (e.g., “My name is John from New York, and my question is…”)
4Ask an actual question
Don’t record a monologue, a treatise, or a screed. if the recording is not a short question, we cannot play it on the show.