contact : 415-925-9404
frequently asked questions

frequently asked questions
There are, understandably, a good number of questions that arise when facing infertility problems. Below we’ve provided answers to those that are most common to the majority of couples considering treatment.
What is infertility?
Infertility is defined as the inability to conceive after 12 months of regularly occurring unprotected intercourse. This time interval is based on the fact that after a period of 1 year, approximately 90% of couples will have conceived. For the remaining 10%, many of those are not infertile but rather subfertile. That is to say, conception can occur, but it might just take longer than average or require medical intervention.
Do I need a fertility specialist?
A fertility specialist, also known as a reproductive endocrinologist, is a physician who has received 2-3 years of additional training past his or her training in general obstetrics and gynecology. Infertility doctors generally focus their work on infertile patients and are well versed at providing complex therapies such as in vitro fertilization (IVF). A variety of factors are involved in deciding whether to consult with a fertility specialist but special consideration should be made for women who are older or have previously failed initial treatments.
What is the relationship between female age and fertility?
Starting in a woman’s late 20’s, fertility begins to slowly decline. After the age of 35-37, this decline accelerates and, by the time a woman reaches her early 40’s, she has only a 5% chance of conceiving each month. For this reason, fertility specialists often recommend seeking treatment after only 6 months of trying if the woman is over 35 years old. Women over 40 should consider consulting with a fertility specialist as soon as they are ready to conceive.
What is male infertility?
Male infertility is defined as any abnormality of sperm count, motility or shape. A semen analysis, a microscopic evaluation of an ejaculated semen specimen, is able to provide information on all of these parameters. There are many causes of sperm production abnormalities including anatomic, hormonal and environmental disruptors. Some causes of male infertility may be treated with medical or surgical interventions while others will require intrauterine inseminations or in vitro fertilization.
What is IUI and when is it performed?
Intrauterine insemination is an office-based procedure where sperm from an ejaculate are washed and concentrated into a small volume that is then deposited into the upper part of the uterus. This positions the sperm closer to where they will meet the egg for fertilization (in the fallopian tube). IUI is often recommended for men with low sperm counts or for couples with unexplained infertility.
What is IVF and when is it performed?
In vitro fertilization (IVF) is a medical procedure that currently offers the best overall chance for conceiving. IVF has multiple steps that take place over a period of several weeks and includes the harvesting of eggs, creation of embryos in the laboratory and placement of those embryos into the uterus. Indications for IVF include tubal factor infertility, male factor infertility and diminished ovarian reserve.
What is ICSI and when is it performed?
Intracytoplasmic sperm injection (ICSI) is a laboratory procedure that facilitates fertilization in certain couples undergoing IVF. The process involves the injection of an entire sperm head into the center of an egg. The egg then undergoes fertilization. Originally developed for men with severe male factor, the indications for ICSI have expanded to include couples with previous fertilization failures during traditional IVF.
Do I need to have fallopian tubes to have a baby?
No. Women who have severely damaged fallopian tubes or have previously undergone a tubal sterilization (and do not want to attempt surgical correction) are still able to have a baby by undergoing IVF.
Is everyone that goes to an infertility specialist recommended to undergo IVF?
Although in vitro fertilization (IVF) currently offers the best chance for conception, this treatment is normally reserved for patients with no other option or for patients who have previously tried other therapies without success. This means that many patients will be candidates for more basic therapies such as superovulation and/or intrauterine insemination. We customarily recommend a stepwise approach to treatment.
Aren’t all infertility evaluations and treatments expensive?
Many patients are surprised to learn that they do have some insurance benefits for fertility such as coverage of the initial consultation. We work closely with ancillary services in the community to provide competitive pricing for fertility testing and, for basic therapies, we have bundled our services at a discounted package price. For more involved therapy, such as IVF, we are pleased to offer package pricing and financing options through CapexMD.
What are donor eggs and when are they recommended?
An egg donor is a woman who donates her eggs to be used by another couple to achieve pregnancy. Egg donation is commonly recommended for women with diminished ovarian reserve, when the chance of conceiving with the use of one’s own eggs is extremely remote. A donor egg cycle is very similar to a traditional IVF cycle but involves synchronization of menstrual cycles between the donor and the recipient (patient).
I’ve been told I have to have IVF, is there any other alternative?
We believe strongly in access to new and experimental treatments. While IVF remains the most successful fertility treatment available, recent advances in our field have added alternative therapies. In vitro maturation (IVM) is an experimental procedure similar to IVF but less laborious and potentially safer for certain patient populations.
What is fertility preservation?
Fertility preservation encompasses interventions designed to counter the effects of other diseases processes or treatments on your reproductive future. One of the most common indications to seek fertility preservation is in the setting of chemotherapy or radiotherapy for cancer patients. Other medical conditions such as infections, inflammatory processes or medications themselves may also threaten fertility.
What can I expect on my first visit?
At your first visit, Dr. Uzelac will take a detailed history and review with you all previous infertility evaluations and treatments. By the end of your consultation you will have a good understanding as to how we approach fertility care and why we are recommending specific tests or treatments for you. We also like to provide you with an overview of what to expect during future office visits. Dr. Uzelac believes that the more information you have access to, the more pleasant and successful your treatment experience will be. Click here for more information on scheduling your initial appointment.
I’ve had my first consultation, what next?
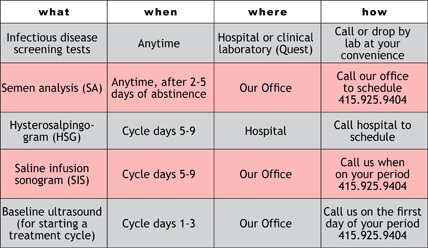
At the conclusion of your initial consultation, a strategy is formulated. Commonly, this will begin with one or more standard evaluations to determine where the problem may lie. For women, many of these tests are scheduled during a specific part of the menstrual cycle. We refer to these specific time points at “cycle days” where cycle day one is the first day of full bleeding. The following is a list of some of the more common tests and how to schedule them: