
contact : 415-925-9404
in vitro maturation

Immature human egg (large circular structure in the middle of picture) surrounded by supportive cells (multiple small circular structures surrounding the egg).
in vitro maturation background and overview
In vitro maturation (IVM) is an evolving infertility treatment that is currently gaining attention as an alternative to traditional IVF. IVM involves the removal of eggs from an ovary before they are fully developed and allowing them to finish their growth process under laboratory conditions. These “in vitro” matured eggs can then be fertilized and used to achieve pregnancy in the same way as in IVF.
In contrast to IVF, IVM use little or no injectable medication called gonadotropins. This dramatically reduces the risk of a treatment complication known as ovarian hyperstimulation syndrome (OHSS). Women at high risk for this complication, such as those with many immature eggs (PCOS), may especially benefit from the IVM procedure.
Limiting the use of gonadotropins during treatment has many additional benefits including lowering the overall treatment cost and reducing the number of office visits during a treatment cycle. Women with aversions to needles or objections to the creation of many surplus embryos (such as may occur in IVF) may also find IVM attractive. Finally, IVM may play an important role in fertility preservation for cancer patients.
IVM frequently asked questions
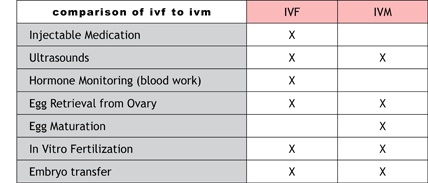
What is the difference between IVM and IVF?
IVF and IVM both involve the removal of eggs from the ovary as part of therapy. While IVF uses injectable medications prior to egg collection, IVM does not. Also in IVM, eggs are collected from the ovary earlier in the treatment cycle than in IVF. All other steps are virtually identical.
What are the major advantages of IVM?
By avoiding excessive ovarian stimulation, IVM virtually eliminates the risk of a potentially serious complication of IVF known as ovarian hyperstimulation syndrome (OHSS). For women at high risk of OHSS, therefore, IVM is the potentially safer therapy. Secondary benefits of avoiding gonadotropins include a reduced treatment cost and a less cumbersome treatment regimen. General side effects associated with gonadotropin usage such as mood changes, bloating or headaches are also avoided in IVM.
What are the major disadvantages of IVM?
IVM cycles have lower pregnancy and implantation rates when compared to IVF. The clinical pregnancy rate for IVM is 30-35% per cycle with implantation rates per embryo of between 10% and 15%. While traditional IVF still offers the best chance to obtain pregnancy (50% per cycle in the best candidates) IVM offers an attractive alternative to those patients who find this treatment prohibitive.
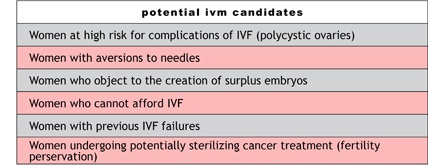
Who are candidates for IVM?
Whereas IVF is used to treat a wide range of fertility disorders, IVM may be best suited for a more select group of individuals. Traditionally, patients at high risk for OHSS have been considered to gain the most benefit from IVM.
Other indications for IVM have been suggested, most of which reflect the simpler and less expensive treatment regimen.
Are children born from IVM healthy?
Unfortunately, worldwide experience in IVM is incompletely documented. Conservative estimates put the number of children born to date with IVM well over 1000. Experience in Canada, Europe, and Asia far surpass that of the United States, however, interest in the procedure here continues to grow. Preliminary reports investigating obstetrical complications, congenital malformations and early childhood development do not suggest any major negative outcomes associated with IVM.
For more information about our IVM program, please contact us at 415.925.9404 or info@marinfertilitycenter.com.
